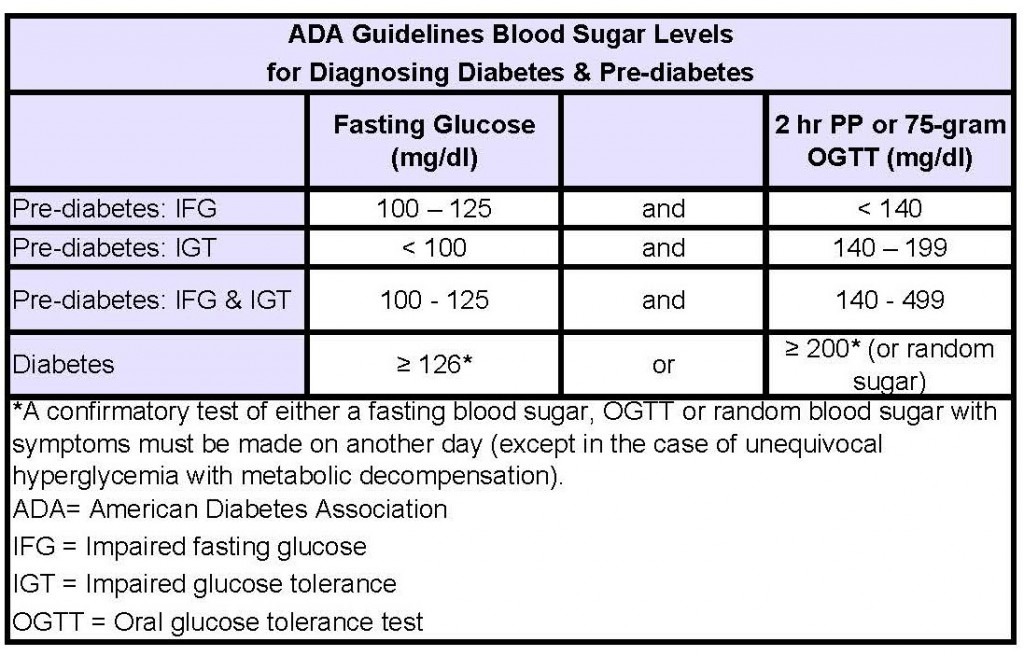
How Type 2 Diabetes is Diagnosed
The hemoglobin A1c test measures the amount of glycosylated hemoglobin (hemoglobin bound to glucose) in your blood and provides information about your average blood glucose levels over the previous 2 to 3 months. Hemoglobin A1c levels over 6.5% are suggestive of diabetes. Another diagnostic test is the fasting blood glucose test. If your fasting blood glucose level is over 126, this establishes that diabetes is present. Random blood glucose levels over 200 are also consistent with diabetes.
Who is most likely to develop type 2 diabetes?
Some groups of people are more likely to develop type 2 diabetes:
-
European 40 years of age or older
-
Diabetes in your family (grandparents, parents, brothers or sisters)
-
Maori, Asian, Middle Eastern or Pacific Island descent aged 30 years or older
-
High blood pressure
-
Overweight (especially if you carry most of your weight around your waist)
-
Diagnosed as having pre-diabetes (also known as impaired glucose tolerance) – this occurs when the glucose (sugar) in your blood is higher than normal, but not high enough to be called diabetes
Warnning Signs Of Diabetes 2
Thirst
Although people with type 2 diabetes may not have specific symptoms, an increase in thirst is one symptom that is characteristic of the condition. The increased thirst can accompany other symptoms like frequent urination, feelings of unusual hunger, dry mouth, and weight gain or loss.
Headaches
Other symptoms that can occur if high blood sugar levels persist are fatigue, blurred vision, and headaches.
Infections
Often, type 2 diabetes is only identified after its negative health consequences are apparent. Certain infections and sores that take a long time to heal are a warning sign. Other possible signs include frequent yeast infections or urinary tract infections and itchy skin.
Sexual Dysfunction
Sexual problems can occur as a result of type 2 diabetes. Since diabetes can damage the blood vessels and nerves in the sex organs, decreased sensation can develop, potentially leading to difficulties with orgasm. Vaginal dryness in women and impotence in men are other complications of diabetes. Estimates suggest that between 35% and 70% of men with diabetes will eventually suffer from impotence. Statistics for women show that about one-third of women with diabetes will have some kind of sexual
Risks You Can Prevent
Certain risk factors related to both lifestyle choices and medical conditions can increase your risk of developing type 2 diabetes. These include:
-
Cigarette smoking
-
Being overweight or obese, especially around the waist
-
Lack of exercise
-
Consuming a diet that is high in processed meat, fat, sweets, and red meats
-
Triglyceride levels over 250 mg/dL
-
Low levels of “good” HDL cholesterol (below 35 mg/dL)
Risks You Can’t Prevent
Some risk factors for diabetes can’t be controlled. Hispanics, Native Americans, Asians, and African Americans have a higher than average risk for getting diabetes. Having a family history (parent or sibling) with diabetes increases your risk. Those over 45 have a higher risk of type 2 diabetes than younger people.
Women’s Risk Factors
Women who developed gestational diabetes in pregnancy have a higher risk for developing type 2 diabetes later in life. The same goes for women who have babies larger than 9 pounds. The insulin resistance associated with polycystic ovary syndrome also places women with this condition at a higher risk for diabetes.
How Does Insulin Work?
Insulin is a hormone that allows the body to efficiently use glucose as fuel. After carbohydrates are broken down into sugars in the stomach, glucose enters the circulation and stimulates the pancreas to release insulin in the proper amount. Insulin allows the uptake of glucose by body cells for use as energy.
Type 2 Diabetes: Insulin Resistance
In type 2 diabetes, the body’s cells cannot take up glucose properly, leading to high levels of glucose in the blood. Insulin resistance means that although the body can produce insulin, the body’s cells do not respond properly to the insulin that is made. Over time, the pancreas reduces the amount of insulin that it produces.
Note the different types of diabetes.
Diabetes affects the way that blood sugar(glucose) is processed in your body. An essential energy source, glucose is present in the bloodstream after digesting food. Insulin, normally produced by the pancreas, assists the glucose out of the blood and distributes it to the liver cells, muscles, and fat, where it is turned into usable energy for the body. There are two types of diabetes: Type 1 and Type 2. Approximately 10 percent of people with diabetes have Type 1, while Type 2 is more prevalent. In brief, the background to the types of diabetes is as follows:
-
Type 1 diabetes: This condition involves destruction of more than 90 percent of the insulin-producing cells of the pancreas, causing the pancreas to cease making insulin or to make very little. Type 1 diabetes tends to occur prior to the age of 30 and it may involve an environmental factor, as well as a genetic predisposition.
-
Type 2 diabetes: While the pancreas continues to produce insulin, or even higher levels of insulin, the body develops a resistance to the insulin, causing scarcity of insulin for the body’s needs and blood sugar levels remain permanently too high. While this type of diabetes can occur in children and adolescents, it usually begins in people over 30 and becomes more common as people age. It tends to run in families and around 15 percent of people over 70 have diabetes Type 2. Type 2 may not show symptoms for years or even decades before being diagnosed, as health may, silently, reach a crisis event before one seeks medical attention. Pay attention to possible indicators…
-
Gestational diabetes develops during pregnancy. Left undiagnosed and/or untreated, serious side effects can injure the mother and affect the unborn child. Having gestational diabetes, that resolves after delivery, increases your chances of developing Type 2 Diabetes in some point of your life and getting gestational diabetes in a next pregnancy. It also increases the chances of getting cardiovascular diseases after 15 to 20 years from 1.5 to 7.8 times!
-
Diabetes due to surgery, drugs, malnutrition, infections, and other illnesses, hereditary disorders that may lead to diabetes (such as cystic fibrosis), may all account for 1 percent to 2 percent of the diagnosed cases of diabetes.Diabetes insipidus is not related to blood sugar levels.It is a relatively rare disease and is not covered in this article.
Skin Problems & Care for Diabetic Skin
About a third of people with diabetes will develop skin problems at some point. In fact, some skin issues can be warning signs of diabetes. The good news is that most skin conditions can be treated easily, if they’re caught early. Keeping proper control of your blood sugar (glucose) can prevent skin problems, and many other diabetes symptoms, from happening in the first place.
Porblems
Localized itching:
Diabetics often experience itchy skin, particularly in the lower legs, which can be caused by dryness, poor circulation, or yeast infections.
Diabetic dermopathy:
Characterized by light brown scaly patches on the shins and legs, diabetic dermopathy (DD) is the most common skin condition associated with diabetes.
Atherosclerosis:
“High blood sugar can cause atherosclerosis, a narrowing of the blood vessels, which results in decreased blood supply to the skin and other areas of the body”
Bacterial and fungal infections:
Diabetics are often more prone to bacterial and fungal infections of the skin, including staphylococcus (staph) infections, yeast infections, and athlete’s foot. “Infections may also occur in skin folds, such as under the arms or the breasts, or less commonly, in the mouth
Necrobiosis:
A skin condition seen almost exclusively in diabetics or people who are insulin resistant, necrobiosis appears as a rash of purple spots, most often on the lower legs and feet.
Acanthosis nigricans:
This condition causes dark patches of thickened, “velvety” skin to develop in areas where there are skin folds, such as the neck, groin, and underarms.
Digital sclerosis:
This diabetic skin condition is marked by thickened, “waxy” skin, usually on the back of the hands and fingers. It can also affect the toes and the back of the neck.
Care
Most skin conditions can be treated or prevented entirely by taking good care of your skin and managing your diabetes responsibly. Try these tips from the American Diabetes Association to keep your skin in good health:
-
Once a week, thoroughly inspect your skin (especially your lower legs and feet) for persistent or unusual sores, bruises, pain, or any other symptoms, and inform your doctor about them at once.
-
Keep your skin clean and avoid chafing by applying talcum powder — especially to such places as the armpits and groin.
-
Avoid very hot baths and showers and use a gentle moisturizer regularly.
-
Don’t scratch! Scratching that itch can create tiny openings in the skin, making you more prone to infection.
-
Don’t smoke. It can worsen several diabetic skin diseases.
-
Wear gardening gloves or work gloves to protect your hands during rough activities, and always wear shoes.
-
See a dermatologist about any skin conditions that you can’t cure on your own.
What Is Type 2 Diabetes?
Type 2 diabetes can affect all people, regardless of age. Early symptoms of type 2 diabetes may be missed, so those affected may not even know they have the condition. An estimated one out of every three people with type 2 diabetes are not aware they have it. Diabetes interferes with the body’s ability to metabolize carbohydrates for energy, leading to high levels of blood sugar. These chronically high blood sugar levels increase a person’s risk of developing nerve problems, vision loss, cardiovascular disease, and other conditions.
Type 2 Diabetes Prevention
Type 2 diabetes is preventable in many cases. At the least, it is possible to reduce the incidence of complications of diabetes by eating a healthy diet, getting moderate exercise, and maintaining a healthy weight. It’s also helpful for people at risk to be screened for diabetes and prediabetes, so that management can begin early in the course of the disease. This reduces the risk of long-term problems.
How do I start treating and managing my type 2 diabetes?
In a nutshell: some people with type 2 diabetes may be able to manage their diabetes through diet and exercise, or by taking tablet medication. However, eventually many people with type 2 will manage their diabetes with insulin as well.
Your doctor will advise you on what treatment is best for you, but whatever this may be, healthy food choices and staying active is important. The goal is to lower your blood glucose and improve your body’s use of insulin. This is achieved through:
-
A healthy diet
-
Exercise
-
Weight loss
The focus of your food choices and regular exercise is to achieve and maintain healthy blood glucose levels. Losing weight helps your body use insulin better. A lot more information about these things can be found in the “Managing Diabetes” section.
You may also have to take medication. Type 2 diabetes is a progressive condition. This means that over time you will gradually produce less and less insulin. Although you may be able to manage your blood glucose levels in the healthy range by eating healthy food and having regular exercise for a number of years, most people come to need tablets or insulin as well as their food and exercise plan.
There is no cure for diabetes. However, treatment aims to keep your blood glucose levels as normal as possible, which will control your symptoms and minimise the risk of health problems developing later on.
If you’re diagnosed with diabetes, you may be referred to a diabetes care team for specialist treatment, or your GP surgery may provide first-line diabetes care.
In some cases, it may be possible to control your diabetes symptoms by making changes to your lifestyle, such as eating a healthy diet and taking regular exercise (see below).
However, as type 2 diabetes is a progressive condition, you may eventually need to take medication to keep your blood glucose at normal levels. You may need to take tablets initially, but move on to injected therapies, such as insulin, at a later stage.
[button color=”red” size=”medium” link=”http://calmingmelody.com/psychologist-glass-water/” target=”blank” ]A Psychologist and a Glass of Water[/button]
[button color=”pink” size=”medium” link=”http://calmingmelody.com/control-blood-sugar-nutrition-fitness/” target=”blank” ]How To Control Blood Sugar With Nutrition & Fitness[/button]


[button color=”green” size=”medium” link=”http://calmingmelody.com/stuffed-cutlets/” target=”blank” ]Stuffed Cutlets[/button]